Today's rapidly evolving healthcare market is leading numerous local hospitals to consider affiliating with larger medical systems.
The decision to affiliate and choosing a partner are likely to be among the most important decisions leadership will make.
Hospitals about to begin or in the middle of the affiliation process can learn from the experience of others. White Plains (N.Y.) Hospital, which finalized its partnership with Montefiore Health System in January 2015, selected Montefiore after a thorough and deliberate process that represented the best strategic thinking of all organizational stakeholders. The story of how we conducted our search, identified our selection criteria, involved key stakeholders and reached a decision should shed light on the process for other institutions.
Choosing to Affiliate
The passage of the Patient Protection and Affordable Care Act led White Plains Hospital to renew and intensify its strategic planning process. Starting in 2010 and continuing through 2013, we began to evaluate the expected changes in the national, state and local markets as a result of the ACA as well as an evolving and more competitive market dynamic.
The rigorous process included a full market environmental review, a SWOT (Strengths, Weakness. Opportunities and Threats) analysis, and a review of stakeholder opinions. For the environmental review, we included a market share analysis, a review of the current competition and the anticipated changes in the competitive landscape, changes in the insurance market, changes in the government programs, and anticipated impact of the ACA on volume, payment, and delivery system innovation.
After evaluating our strategic vision and business imperatives, it became clear that a comprehensive partnership would be key to our future success. Over the past six years, White Plains Hospital has increased its range of tertiary level services. We opened a cardiac catheterization laboratory and enhanced our thoracic and vascular surgery programs, among many other things. As we looked toward the future, it became increasingly clear that ambulatory and less acute care would rapidly shift to outpatient settings, and the more complex, chronic and critical care would occur in the inpatient hospital settings. Therefore, a major component of our affiliation discussions would explore which academic center was truly dedicated to commit the resources to enhance the tertiary services at White Plains Hospital as a regional focal point for their health system.
As we analyzed the wave of market changes driven by the federal government, it also became clear that there would be fundamental changes in how care providers are compensated. Traditionally, hospitals have been responsible for the care and results inside hospital walls. However, compensation models increasingly include after care and readmissions. Therefore, hospitals will need systems in place for "population health," or care management beyond the hospital walls. It was crucially important to affiliate with a larger system that would assist us with this.
We also anticipated needing access to greater capital at reasonable cost to meet increasing demand for more complex services. An affiliate that could provide access to capital in a cost effective manner seemed necessary.
Although our strategic vision is to deliver exceptional care at the local level, we perceived an increased need to deliver it through a scaled infrastructure, not only through back office and corporate services, but by also participating in more innovative and creative insurance contracting opportunities. In terms of clinical services, scaled infrastructure would allow for the delivery of more complex innovative care.
Finally, although our quality performance is among the highest in New York State, we decided that affiliating with a major academic medical center with ample clinical resources would enhance our ability to maintain and improve our performance.
Analyzing existing relationships
For 17 years, White Plains Hospital had been part of Stellaris, a local health system comprising four community hospitals. In addition, we had a 20-year clinical affiliation with a large academic medical system. Our SWOT analysis created an excellent framework to critically evaluate our existing relationships and whether they were strategically aligned with our vision of the future.
Since 1997, our relationship with Stellaris had provided real and lasting value, particularly from an economic viewpoint. It enabled us to create an electronic medical record system and meet meaningful use regulations. It also helped us to gain a HIMSS level 6 designation. In addition, we were able to jointly develop a quality-monitoring system that qualified us to negotiate major pay-for-performance contracts and established us as top performers in publicly reported quality evaluations. There were numerous other programs that provided value, including operating an ambulance company, setting up a captive insurance company and jointly contracting for employee health benefits.
However, the anticipated market changes we identified called for a different type of partner than what existed with Stellaris.
In parallel, we evaluated the academic medical center relationship. This affiliation began in the early 1990s as a teaching relationship. It grew to include a cardiac catheterization program, neonatal transfer coverage, pediatric surgery and psychiatric coverage. As we expanded tertiary-level services to provide the complex, chronic and critical care that account for more inpatient care, we knew we needed an academic center truly dedicated to committing resources to enhance our hospital's tertiary services We concluded that we needed to seek out other academic medical center partners that would consider us as a regional focal point for a growing health system.
Bringing it to the board
Once we reached the conclusions regarding our current partners, it was important to have a candid discussion with our board of directors and propose a recommended process to evaluate potential partners. Our board chair appointed an ad-hoc affiliation committee, which represented the board leadership, medical leadership and senior management.
We conducted research to start the process and identify likely affiliation candidates. We profiled the major systems in the New York metropolitan area and reached out to major national systems. It quickly became clear to us that the national systems were not going to be likely candidates because they were focused on the local markets they currently served. We identified six potential candidates in our region: Montefiore Health System, Mount Sinai Health System, New York-Presbyterian Healthcare System, North Shore-LIJ Health System, NYU Langone Medical Center and Yale New Haven Health System. Our evaluation looked at their size, financial performance, quality scores, strategic plans, readiness to implement population health strategies and numerous other evaluations.
White Plains Hospital's president and its chief executive officer contacted the candidates. We met with them on their campuses for half-day fact-finding meetings and then invited them to meet on our campus for another half-day. In each case, we met with the CEO, system executive, chief medical officer and other leaders. The meetings were helpful and instructive, and the scope of the discussions was wide-ranging.
While we were scheduling the meetings, we also continued two pieces of important work. The first was to create a list of evaluation criteria to apply to each potential affiliate and second was to establish what we wanted from a relationship, including governance structure, strategic alignment, access to capital, physician engagement, preparation for health reform and efficient corporate services, among other components. We also recognized that our medical staff is a key stakeholder in this process and scheduled two meetings with active physicians to discuss the affiliation process, candidates and strategy. These meetings were lively and very helpful. Throughout everything, there were periodic updates to the entire board to keep everyone in the loop.
The affiliation committee agreed to retain financial and legal counsel, as the board of directors needed to be fully educated to the different legal structures and options available in creating an affiliation with a larger system. The legal advisors prepared an analysis of the different legal structures that could shape the affiliation agreement and future governance of the hospital.
Choosing the corporate structure
One of the most important discussions we had with our board leadership was the available corporate structure or governance options, which were laid out by our legal advisors.
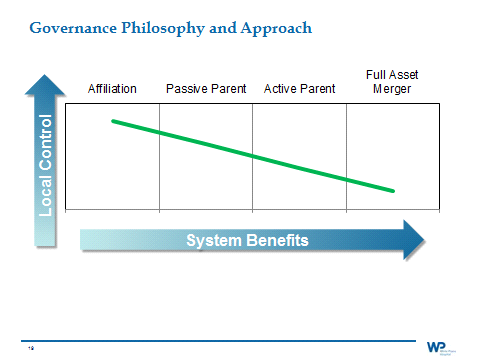
These options included an affiliation, a passive parent structure, an active parent structure or a full asset merger. We sought the advice of our corporate legal counsel to understand the implications from governance and operating perspectives.
It became clear that the opportunity to capture more meaningful benefits required reduced local control. If we were serious about meeting our strategic goals, then we had to seriously consider a corporate parent relationship. We fairly quickly eliminated the options of affiliation (due to the lack of real tangible benefits) and a full asset merger (due to the lack of local input). That decision left us with an active or passive parent relationship. Our final conclusion was that the active parent was not that different from the passive parent, but providedmany more potential benefits and flexibility.
Our next issue was to determine to what extent local control was legally possible and operationally practical. Our board of directors is made up of community leaders who take their roles and responsibilities seriously, actively providing policy direction and assisting management in an extremely effective partnership. The key was to preserve what was successful and layer on capabilities and resources to enhance the strategic direction of the organization. We concluded that the existing board should have an important and significant role in setting the strategy and policy direction for the future, and that management should report to the local board for local operations, and report to both the local and the system board in matters of community and system concerns. In addition, the system board should have approval rights over the selection of the local board members and management. This balance would create a true partnership and maximize the capabilities of the existing structure while taking advantage of the larger and broader opportunities.
After we had identified the governance and operating structures we found desirable, we focused on determining our evaluation criteria. An important criterion was continuing to work with our community physicians, with whom we have a long history of effective collaboration and joint decision-making, as key partners in everything we did. Our prospective partner needed to offer opportunities to complement the existing relationships and enhance our ability to effectively structure broader options and opportunities with our physicians.
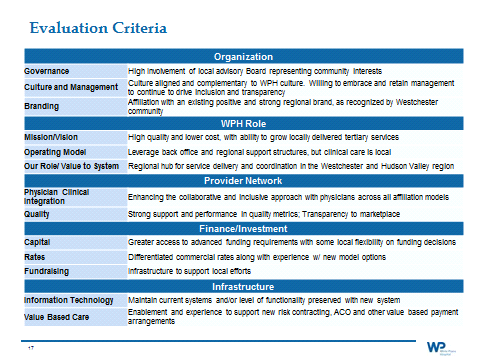
The table above summarizes the criteria and a description of what we attempted to accomplish in the process. Another way to summarize the criteria is as follows:
- Establish White Plains Hospital as the regional tertiary hub for the Westchester County market;
- Enhance opportunities to build upon the partnerships with local physicians;
- Create access to capital to support the facilities and evolution of the campus revitalization;
- Access economies of scale to remain cost competitive; and
- Create the support for successfully dealing with changes initiated by health reform and the evolving competitive landscape.
After we determined the desirable governance state and the criteria for evaluation, we drafted the RFI. The intention was to ask each potential affiliate to respond in writing and address the criteria that were important to White Plains Hospital. We requested responses within a tight time frame (30 days).
Five of the six academic centers responded. New York Presbyterian declined to respond as they had previously signed an exclusive relationship with a competitive hospital in the Westchester County market.
Each of the five submissions was well done and thorough. They all answered our questions and made excellent cases for the development of a relationship with them. Each one had a different approach. The financial consultants summarized the RFI responses and presented them to the committee.
After reviewing the summary, our affiliation committee determined that we should not exclude any of the potential affiliates from further discussions. We agreed to conduct an onsite interview with each potential partner. We also decided that the next step would be to invite the leadership of each academic center to meet the full committee over dinner, followed by an evening discussion. We asked each potential affiliate to bring their chief executive officer, chief medical officer, board chair and anyone else they thought would add to the discussions. We also asked our advisors to sit in (but not participate) so they could help us during our deliberations.
The dinner meetings occurred within a couple of weeks and all were very positive. We again had our consultants summarize the specific discussion and responses. After reviewing the documentation, the committee narrowed the field to three candidates. Two candidates were eliminated for three reasons: (1) a lack of clear consistent strategic alignment; (2) no well-defined access to capital and (3) a different cultural approach than ours.
The remaining three potential organizations seemed to have a strategic alignment, compatible culture and willingness to provide a capital investment into ongoing projects. However, we had unanswered questions and wanted to clarify and document representations made during the dinner meetings. In addition, we felt it was time to draft a proposed Letter of Agreement (LOA) to again make sure were all on the same page.
In the follow up process, one participant dropped out as they decided that the structure we proposed was not consistent with their strategic initiatives.
In the case of the two remaining academic medical centers we conducted a comparative review of each of the criteria and scored each contender as follows:
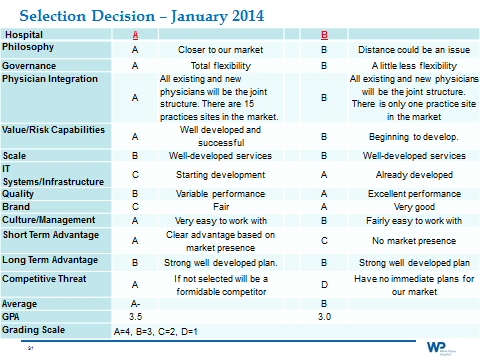
As you can see they came out very close. It then came down to a subjective evaluation based on all the interactions and a feeling as to which organization would be the most compatible.
We drafted an expanded LOA and term sheet. Our selected partner Montefiore Health System worked well with us in negotiating the details of the agreement, and our affiliation committee, our executive committee and our board of directors approved it in the space of two weeks. We felt it was key to have a LOA that reflected as much detail and as many specifics as possible.
The next step was to draft definitive agreements as well as conduct a "due diligence" process. We set aggressive time frames for this work and completed all of it within the deadlines set – approximately 90 days.
As we reflect on this grueling and time consuming process there are several "takeaways" that are important:
- Have strategic planning drive the process. A well-thought-out strategic planning process should be the foundation of an affiliation process;
- Make sure the participants in the process include all stakeholders. The oversight committee should include board and medical and administrative leaders. The individuals involved should commit to spend substantial time on the process and participate in all critical meetings;
- Commit to continuous communication with other board members, medical staff, and other stakeholders. The process can be lengthy and detailed. It is key that other stakeholders are kept current on the process and decision making.
- Assure an organized structured process. Choosing an affiliation partner is most likely the most important decision a board of directors will make in the life of the hospital. The evaluation should be surrounded by a structured organized process that ensures all critical elements are explored;
- Use legal and process consultants. The use of consultants is important as advisors, but they should not drive the process. They can provide background information and keep track of the process;
- Identify priorities that will drive the final decision. The committee needs to decide what are the most important things they seek in an affiliation relationship;
- Senior managers are the experts and should lead the process. Senior management has the experience and understanding of the industry and strategy to drive the process;
- Make sure all representations are in writing. In order to make sure there is no misunderstanding, it is critical that all important transaction components are represented in writing;
- The Letter of Agreement should be as detailed as possible in order to avoid misunderstanding later in the process;
- Make sure you feel comfortable with the culture and management structure. If there is more than one contender, the expectation of which culture and management structure will "fit" the best is key to future success.
Jon B. Schandler is CEO and Susan Fox is the president of White Plains Hospital.
The views, opinions and positions expressed within these guest posts are those of the author alone and do not represent those of Becker's Hospital Review/Becker's Healthcare. The accuracy, completeness and validity of any statements made within this article are not guaranteed. We accept no liability for any errors, omissions or representations. The copyright of this content belongs to the author and any liability with regards to infringement of intellectual property rights remains with them.


